Ligamentum flavum hypertrophy is a complex sounding term that refers to thickening and enlargement of the ligamentum flavum, a ligament found within the spinal column. The severity of this conditions really depends on the degree of thickening. Mild thickening will often cause no symptoms at all, whereas significant thickening can compress the spinal cord and nerve roots, potentially causing pain and other neurologic abnormalities. To better understand the implications of ligamentum flavum hypertrophy, we will take a deeper dive into this condition and discuss is potential impact on your health.
Understanding Ligamentum Flavum Hypertrophy
The ligamentum flavum is a strong, elastic ligament that runs along the back of the spinal canal, connecting the vertebrae. Its main function is to support the spinal column and maintain stability. However, over time or due to certain factors, this ligament can undergo hypertrophy, a process in which it thickens and becomes enlarged. Ligamentum flavum hypertrophy is commonly associated with age-related changes, spinal degeneration, and wear and tear.
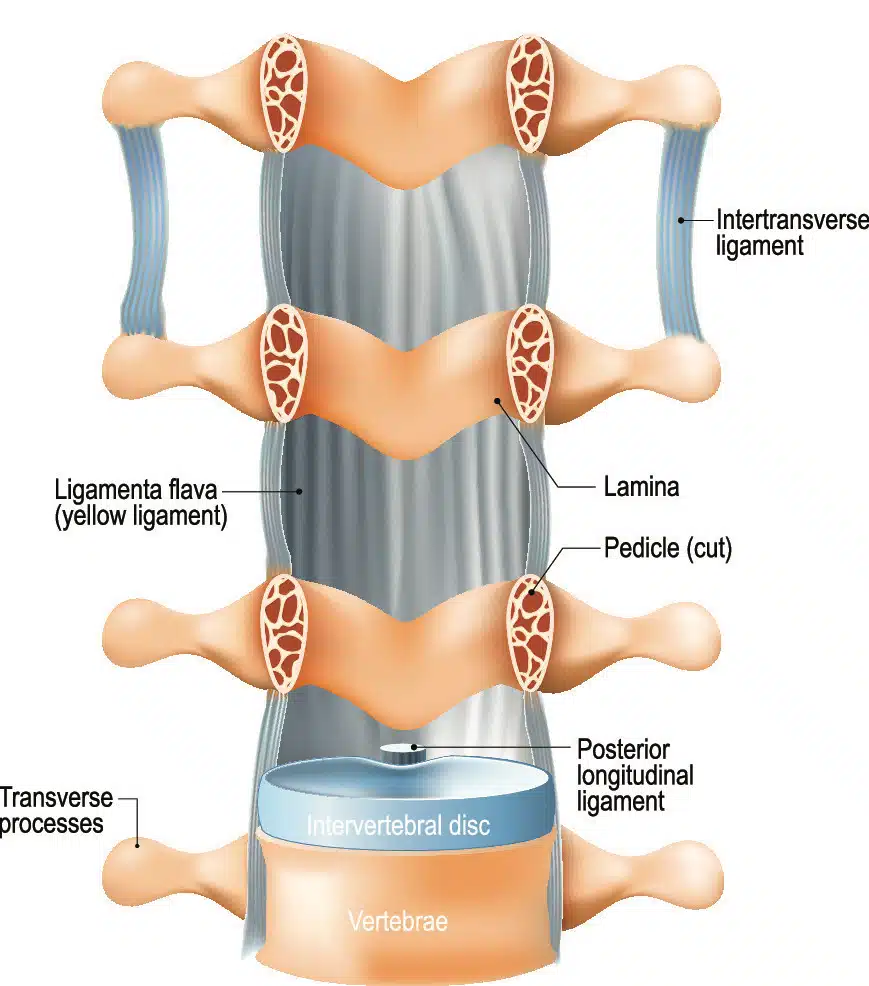
Symptoms and Manifestations
The severity of ligamentum flavum hypertrophy varies from person to person. In some cases, individuals might experience no symptoms at all, while in others, the condition can lead to significant discomfort. Common symptoms include:
- Back Pain: Enlarged ligamentum flavum can contribute to chronic lower back pain, especially in the lumbar (lower) spine.
- Nerve Compression: As the ligament thickens, it can compress nearby spinal nerves, causing symptoms such as radiating pain, numbness, tingling, or weakness in the legs.
- Limited Mobility: Hypertrophy might restrict the spine’s flexibility, leading to reduced range of motion.
Severity Assessment and Complications
The severity of ligamentum flavum hypertrophy is often determined by the extent of ligament enlargement, its impact on nearby structures, and the resulting symptoms. Mild cases might not require immediate intervention, while more pronounced hypertrophy can lead to more severe symptoms and complications if left untreated. Complications might include:
- Neurological Deficits: Nerve compression resulting from hypertrophy can lead to long-term neurological deficits if not addressed promptly.
- Chronic Pain: Persistent pain and discomfort can significantly affect an individual’s quality of life, leading to reduced mobility and overall well-being.
- Functional Limitations: Severe cases of hypertrophy can limit daily activities and hinder an individual’s ability to perform routine tasks.
Treatment Options
The approach to treating ligamentum flavum hypertrophy depends on the severity of symptoms and their impact on the patient’s life. Treatment options include:
- Conservative Measures: For mild cases, conservative treatments like physical therapy, pain management, and anti-inflammatory medications may be recommended to alleviate symptoms.
- Epidural Steroid Injections: Injections of anti-inflammatory medications can help reduce pain and inflammation caused by nerve compression.
- Surgery: In cases where symptoms are severe and conservative treatments are ineffective, surgical intervention, for example a discectomy, might be considered to relieve nerve compression and restore spinal stability.
Conclusion
The severity of ligamentum flavum hypertrophy can vary widely, from asymptomatic cases to those causing significant discomfort and impairment. Individuals experiencing symptoms related to this condition should seek medical evaluation to determine the appropriate course of action. Early diagnosis and a tailored treatment plan can help manage symptoms, prevent complications, and improve overall quality of life. It’s important to remember that each case is unique, and consulting with healthcare professionals is essential to address concerns and make informed decisions about managing ligamentum flavum hypertrophy effectively.