Summary
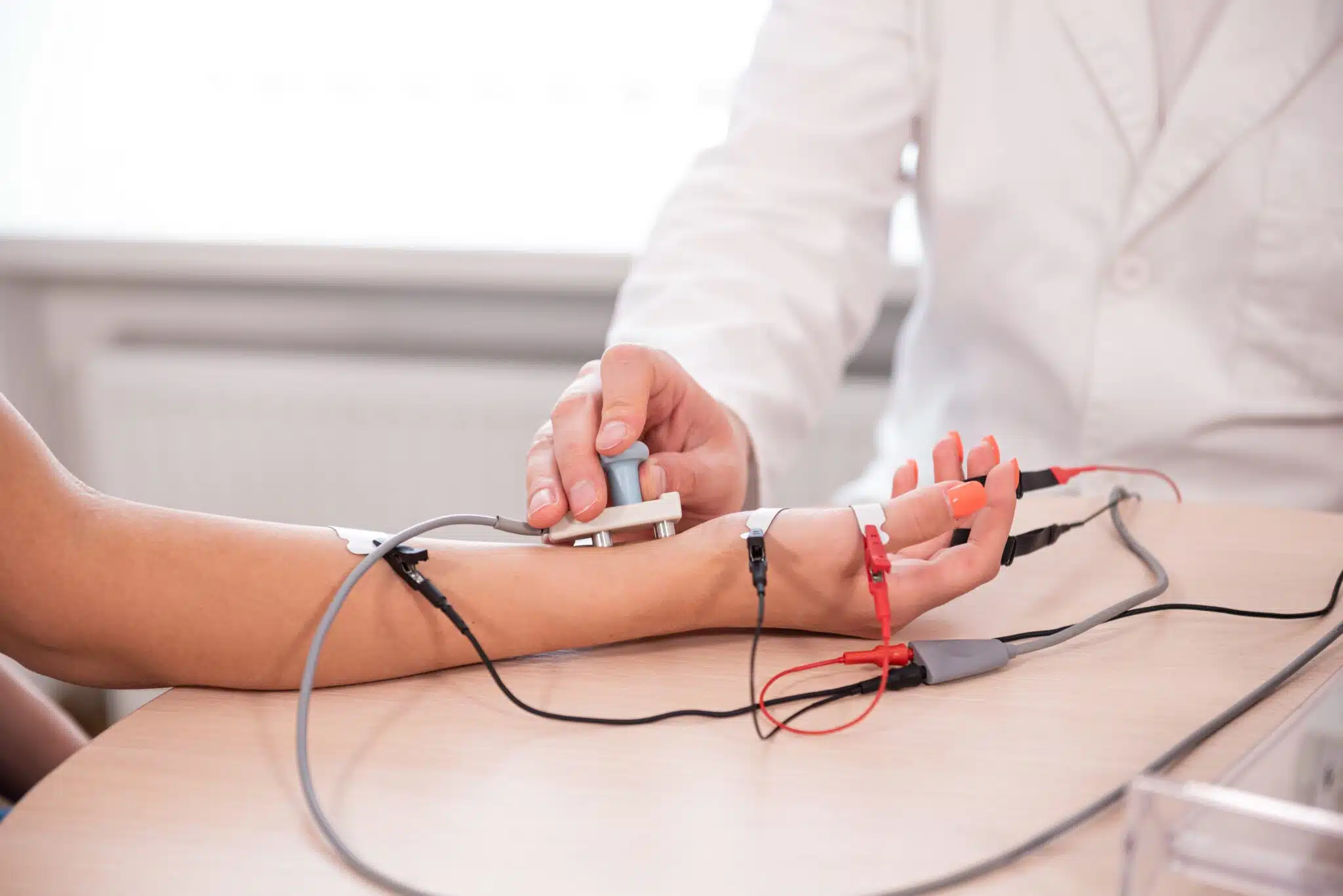
Electromyography (EMG) is a non-invasive diagnostic procedure that helps doctors evaluate the health and function of your muscles and nerves. It involves the use of electrodes that are placed on the skin or inserted into the muscle to detect and measure the electrical signals generated by muscle fibers during contraction and relaxation.
The procedure takes about 30 minutes to an hour and is used to diagnose muscle disorders, nerve injuries, and certain neurological disorders.
What is an EMG?
An electromyography (EMG) is a diagnostic procedure used to evaluate the electrical activity of muscles and the corresponding nerve signals that control them. It provides valuable information about the health and functioning of your muscles and nerves.
During an EMG, small electrodes or fine needles, called electrodes, are placed on or inserted into specific muscles in the area being examined. These electrodes detect and record the electrical signals generated by your muscles when they contract or relax. The recorded signals are displayed on a monitor or recorded for further analysis.
When is an EMG Study Used?
Electromyography (EMG) is a diagnostic procedure used to assess the electrical activity of muscles and nerves. It is often performed in conjunction with nerve conduction studies (NCS), which measure the speed and strength of electrical signals as they travel along a nerve. Together, EMG and NCS provide valuable insights into the functioning of our neuromuscular system and help diagnose various conditions.
Assessing Neuromuscular Disorders
EMG plays a crucial role in diagnosing and managing neuromuscular disorders. By analyzing the electrical signals produced by muscles, it helps healthcare professionals identify abnormalities and provides valuable information about conditions such as muscular dystrophy, myasthenia gravis, amyotrophic lateral sclerosis (ALS), peripheral neuropathy, and other muscle or nerve-related disorders.
Identifying Nerve Entrapment and Compression
EMG is a valuable tool in identifying nerve entrapment or compression syndromes, which commonly occur in conditions like carpal tunnel syndrome, cubital tunnel syndrome, and radiculopathies (pinched nerves) such as sciatica. By pinpointing the affected nerves and assessing the severity of the condition, EMG aids in appropriate treatment planning.
Assessing Nerve and Muscle Injuries
EMG helps evaluate nerve and muscle injuries and monitor their recovery progress. By determining the extent of nerve damage and distinguishing between nerve and muscle involvement, EMG assists healthcare providers in formulating tailored treatment strategies.
What to Expect During the Test
If your healthcare provider has recommended an electromyography (EMG) test, it’s natural to have questions and concerns about what to expect. We’ll discuss the typical steps involved below.
Preparing for the EMG
Before the EMG, your healthcare provider will provide specific instructions to ensure a successful test. These may include avoiding lotions or creams on your skin, discussing any medications you are taking, and informing them of any bleeding disorders or implanted medical devices.
The EMG Procedure
- Placement of Electrodes: During the EMG, you will be comfortably positioned, either lying down or seated. The healthcare professional will place small, adhesive electrodes on your skin over specific muscles or insert fine, sterile needles into targeted muscles. The number of electrodes or needles used depends on the area being tested.
- Muscle Activity Assessment: Once the electrodes or needles are in place, the healthcare professional will ask you to relax or contract specific muscles. As you do so, the EMG machine will detect and record the electrical signals generated by your muscles. This process helps evaluate muscle activity and detect any abnormalities.
- Completion of the Test: Once the required data is collected from the muscles and nerves being examined, the electrodes or needles will be removed. You may experience slight discomfort during needle removal, similar to a quick pinprick.
How Long Does the Study Take?
The length of the EMG procedure varies depending on the area being tested. It can last anywhere from 30 minutes to an hour.
Does it Hurt?
While some individuals may find certain aspects of the test mildly uncomfortable, such as the insertion of needles or the brief electrical impulses, the discomfort is generally minimal and temporary.
Who Should Avoid EMG?
In general, electromyography (EMG) is a safe procedure that can provide valuable diagnostic information. However, there are certain situations where caution or avoidance of an EMG may be necessary.
- Bleeding Disorders: If you have a bleeding disorder or are taking blood-thinning medications (such as warfarin or aspirin), your healthcare provider may need to evaluate the risks versus benefits of an EMG. They may suggest alternative testing methods or adjust your medication regimen prior to the procedure to minimize bleeding risks.
- Skin Infections: If you have an active skin infection or an open wound in the area where the EMG electrodes or needles would be placed, it may be necessary to postpone the test until the infection has resolved. Performing the EMG in such circumstances could potentially worsen the infection or introduce bacteria into the deeper tissues.
- Implanted Devices: If you have certain types of implanted devices such as pacemakers, defibrillators, or deep brain stimulators, special precautions may need to be taken. EMG involves the use of electrical signals, which can potentially interfere with the functioning of these devices. Your healthcare provider will coordinate with the appropriate specialists to determine if an EMG is safe or if alternative diagnostic methods should be considered.
- Pregnancy: Although EMG is generally safe during pregnancy, it is recommended to discuss the potential risks and benefits with your healthcare provider. They can provide guidance based on your specific situation and determine if any modifications or precautions are necessary.
Final Thoughts
Overall, EMG is a valuable tool that provides important information for diagnosing and managing various conditions affecting muscles and nerves. By understanding the procedure and potential considerations, we hope you feel more informed and prepared when undergoing this diagnostic procedure.