Degenerative disc disease (DDD) is a common condition in which the intervertebral discs in the spine break down and deteriorate, usually due to age-related wear and tear. The intervertebral discs act as cushions between the vertebrae in the spine, helping to absorb shock and allow the spine to move freely. In degenerative disc disease, these discs may become thinner, weaker, or less flexible, which can cause pain and stiffness. Treatment for degenerative disc disease may include medications, physical therapy, and, in some cases, surgery.
Definition
Degenerative disc disease (DDD) is a condition in which the intervertebral disc deteriorates and becomes thinner, weaker, and less flexible.
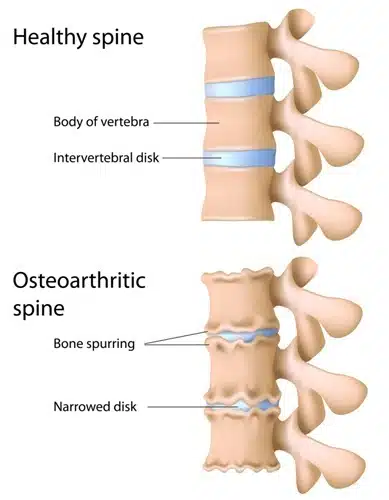
The spine is made up of a series of bones called vertebrae, which are stacked on top of each other and separated by intervertebral discs. These discs are made up of a tough, outer layer called the annulus fibrosus and a softer, gel-like center called the nucleus pulposus.
The intervertebral discs serve several important functions in the spine. They act as cushions between the vertebrae, helping to absorb shock and allowing the spine to move freely. They also help to distribute weight and load evenly across the spine.
In degenerative disc disease, the gel-like nucleus can dry out and the fibrous outer layer can become brittle, causing the disc to shrink or break down.
Prevalence
Degenerative disc disease is a common condition and its prevalence increases with age. By the age of 20, 37% of people show signs of disc degeneration on imaging. By the age of 70, that number increases to 93%.
Causes
There are several factors that can contribute to the development of degenerative disc disease:
- Aging: Degenerative disc disease is more common in older adults, as the discs in the spine naturally dry out (desicate) and become less flexible and less able to absorb shock over time.
- Genetics: Some people may be more prone to developing degenerative disc disease due to their genetics.
- Occupation or activities: Certain occupations or activities that involve repetitive motions or heavy lifting may put extra stress on the spine and increase the risk of degenerative disc disease.
- Injury: Traumatic injuries to the spine, such as a car accident or sports injury, can damage the intervertebral discs and lead to degenerative disc disease.
Symptoms
The symptoms of degenerative disc disease may include:
- Pain: Pain is the most common symptom of degenerative disc disease. It can range from a dull ache to a sharp, shooting pain. The pain may be worse when sitting, standing, or walking for long periods of time. It may also be worse when bending, lifting, or twisting the back.
- Stiffness: People with degenerative disc disease may experience stiffness in the back or neck. This may be worse in the morning or after periods of inactivity.
- Limited range of motion: Degenerative disc disease may cause difficulty with certain movements, such as bending, twisting, or reaching.
- Weakness: Some people with degenerative disc disease may experience weakness in their legs or arms if there is associated nerve compression.
- Numbness or tingling: Degenerative disc disease may cause numbness or tingling in the arms, hands, legs, or feet if there is associated nerve compression.
It’s important to note that these symptoms can also be caused by other conditions, and it’s always best to see a healthcare provider for a proper diagnosis.
Diagnosis
There are several tests that a doctor may use to diagnose degenerative disc disease. These may include:
- Physical examination: During a physical examination, the doctor will examine your spine and evaluate for tenderness, stiffness, or limited range of motion that may suggest degenerative disc disease.
- Magnetic resonance imaging (MRI): An MRI uses a powerful magnetic field and radio waves to create detailed images of the inside of your body, including the bones and soft tissues of your spine. An MRI can help the doctor see if there is any damage or degeneration of the discs.
- Discography: In a discography, a small amount of dye is injected into one or more of the discs in your spine. This dye can be seen on an X-ray, which can help the doctor see if there is any damage to the discs.
It’s important to note that these tests may not be necessary for everyone. Your doctor will consider your specific symptoms and medical history to determine which tests are appropriate for you.
Treatment
The treatment of degenerative disc disease typically depends on the severity of the condition and the degree of pain being experienced. Some common treatment options for degenerative disc disease include:
- Medication: Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or naproxen can help reduce pain and inflammation. In more severe cases, the doctor may prescribe stronger pain medications, such as opioids or muscle relaxants (which should be used with caution).
- Physical therapy: Physical therapy can help strengthen the muscles of the back and improve flexibility and range of motion. A physical therapist may also teach you exercises to help reduce pain and improve posture.
- Injections: Corticosteroid injections around an irritated nerve can decrease inflammation and improve pain. Other newer therapies, such as plasma injections, can be injected directly into the intervertebral discs. These also include Growth Factors and Stem Cells that decrease inflammation and delay degeneration.
- Surgery: In severe cases of degenerative disc disease that do not respond to other treatments, surgery may be necessary. Options may include disc removal or replacement (discectomy), spinal fusion, or laminectomy (removal of a portion of the vertebrae to relieve pressure on the nerves).
It’s important to note that treatment options may vary depending on the individual’s specific condition and overall health. It’s important to discuss all treatment options with a doctor to determine the best course of treatment for your needs.
Sources
Kalichman L, Cole R, Kim DH, et al. Spinal stenosis prevalence and association with symptoms: the Framingham Study. Spine J. 2009;9(7):545-550. doi:10.1016/j.spinee.2009.03.005
Romaniyanto et al. “An update of current therapeutic approach for Intervertebral Disc Degeneration: A review article.” Annals of medicine and surgery (2012) vol. 77 103619. 15 Apr. 2022, doi:10.1016/j.amsu.2022.103619