Summary
Spinal stenosis refers to the narrowing of canals within the spinal column. This narrowing may be due to a variety of causes such as degenerative changes, herniated discs, trauma, or tumors. When the spinal canal or other smaller canals narrow, this may compress the spinal cord or other nerves. This can result in pain as well as numbness and weakness in the arms or legs (depending on the location of stenosis). Treatments depend on the underlying cause and include medications, physical therapy, and in severe cases, surgery.
Definition
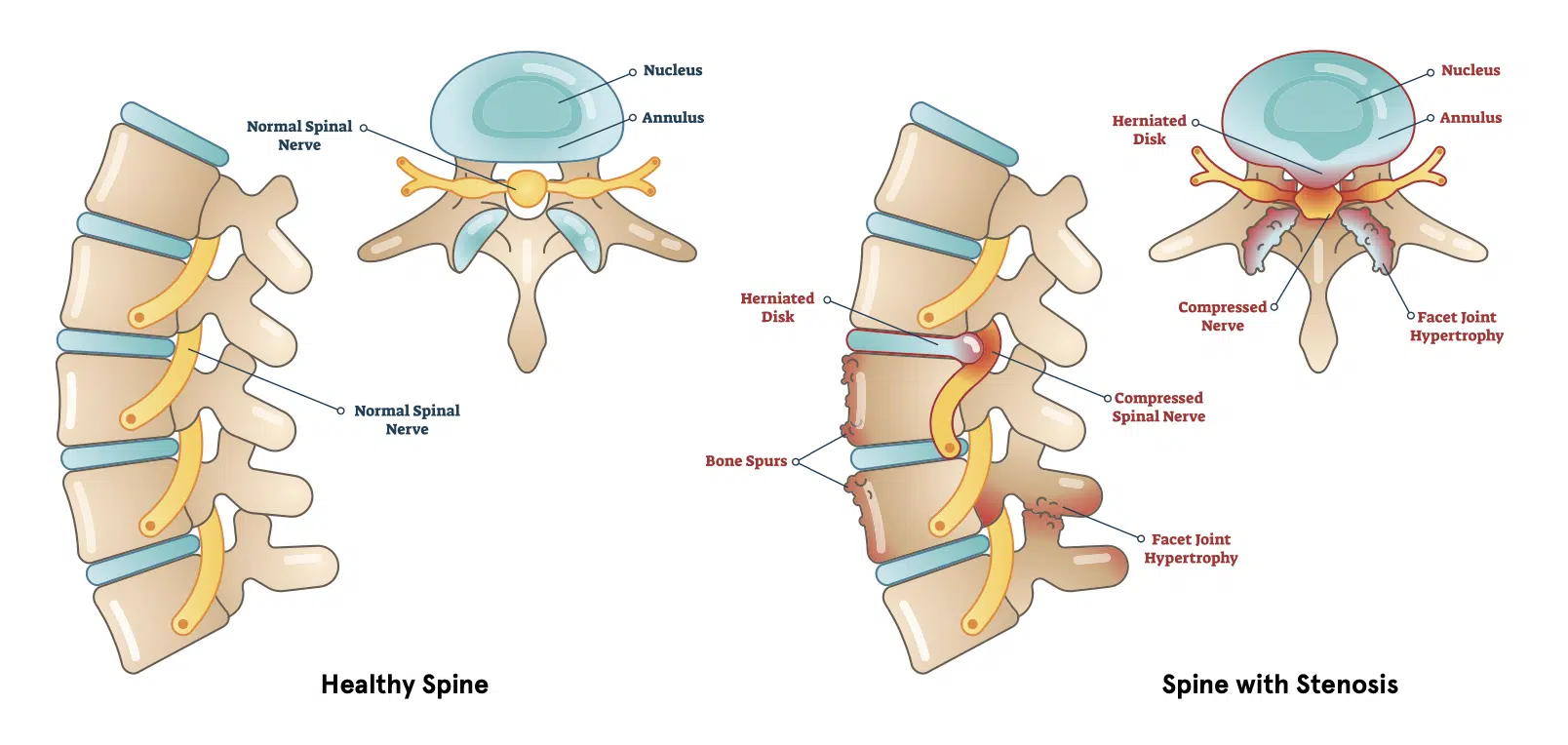
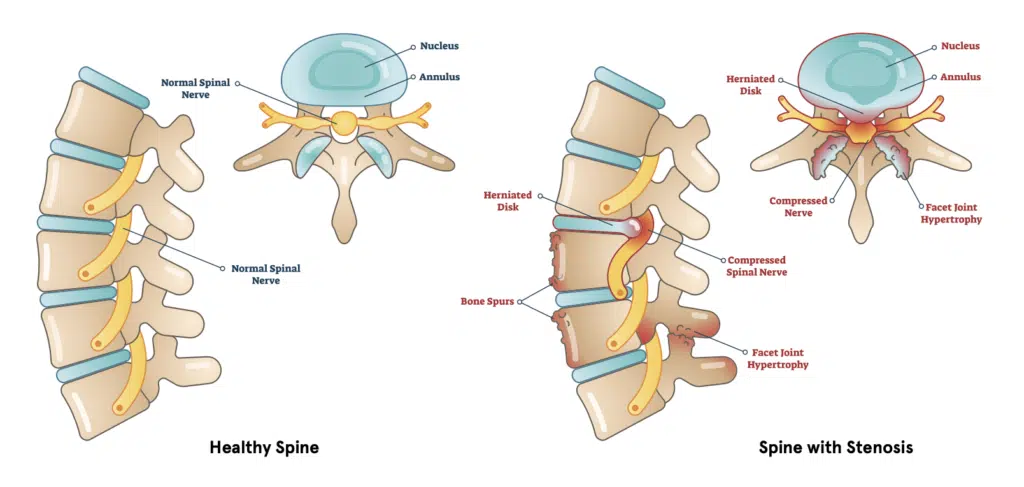
The spinal column is made up of 33 bones, called vertebrae, which are separated by intervertebral discs. One of the main functions of the spinal column is to protect the spinal cord and the nerves which branch off it. The spinal cord runs through the central canal and nerves which branch off from the cord exit through the neural foramina. Spinal stenosis is a condition in which there is narrowing of one or more of these canals.
Prevalence
The prevalence of spinal stenosis ranges from 11% to 38% of the population and increases with age.
Causes
Spinal stenosis is a general term referring to narrowing of spinal canals. There are many potential causes for canal narrowing. Some example conditions are below:
- Degenerative changes: General wear and tear and age related changes can cause narrowing of the canals. Osteophytes, also known as bone spurs, are bony overgrowths seen in arthritis. Thickening of the ligaments which hold the bones together, known as ligamentum flavum hypertrophy, is another cause of stenosis from degenerative changes.
- Herniated disc: A herniated disc, also known as a slipped disc or a ruptured disc, is a condition in which the outer layer of a disc (annulus) breaks and the gel-like contents (nucleus pulposus) leaks into the canal.
- Congenital: Congenital spinal stenosis refers to narrowing that is present at birth.
- Spondylolisthesis: Spondylolisthesis is a condition in which the vertebra slips out of place in relation to the one above. This can be due to degenerative change or as the result of trauma.
- Trauma: A fracture of the vertebra may change the structure of the canal or result in bone fragments migrating into the canal causing stenosis.
- Tumors: Tumors or abnormal growths, which may be cancerous or benign, can cause narrowing of the spinal canal.
- Infection: An infection can result in the accumulation of pus, called an abscess, which can cause canal narrowing.
Symptoms
The symptoms of spinal stenosis depend on the location and severity of canal narrowing. The symptoms are the result of either the spinal cord or the spinal nerves being compressed as a result of the narrowing.
If the stenosis is present in the cervical spine (neck) then symptoms may include:
- Neck pain
- Shoulder or arm pain
- Arm numbness
- Arm weakness
If the stenosis is present in the lumbar spine (low back), then symptoms may include:
- Back pain
- Buttock pain
- Leg pain
- Leg numbness
- Leg weakness
Symptoms of bowel or bladder incontinence, numbness in the private parts, or weakness in both legs are signs of severe disease and a dangerous condition known as cauda equina syndrome. It is important to immediately seek medical attention if any of these symptoms are present.
Diagnosis
Often the diagnosis can be made clinically, meaning based on detailed interview and a careful physical examination. However, sometimes more studies are needed based on the assessment or if symptoms do not improve after initial visits.
Imaging studies such as x-ray, CT scan, and MRI, are commonly used to make diagnosis. Each visualizes different body parts and has it’s own strengths and weaknesses.
- X-ray – uses the passage of electromagnetic waves to create shadow like images of bones and some organs. X-rays are quick and accessible but do a poor job evaluating soft tissues such as discs, muscles and nerves.
- CT scan – also known as Computed Tomography, uses a series of x-rays along with computer processing to create detailed cross-sectional images. CT scans produce higher quality images however they are associated with more radiation exposure.
- MRI -which stands for Magnetic Resonance Imaging, uses a magnetic field and radio waves to create images of the body. MRI does a great job of visualizing tendons, ligaments, nerves, and intervertebral discs. Another benefit is that there is no radiation exposure. Unfortunately, MRI’s often are associated with longer wait times and higher cost.
Treatments
Treatment for spinal stenosis should take into consideration the underlying cause. Typically a stepwise approach to treatments is taken, starting with the least invasive treatments (medications and physical therapy) to the most invasive (surgery).
- Medications: – Medications can either be taken orally (by mouth) or applied topically (on the skin). Non-steroidal anti-inflammatory medications (NSAIDs), such as ibuprofen, are common first line treatments. More severe pain may be treated with opioids or muscle relaxants with extreme caution. Topical medications, which can be applied on the skin, include capsaicin cream or lidocaine patches.
- Exercise & Physical Therapy: Directed exercises and physical therapy can help stabilize the spine, improve pain, and enhance flexibility. Some people may also find that yoga is helpful in managing their symptoms.
- Epidural Steroid Injections: Epidural steroid injections (ESI) and facet joint injections are more invasive treatments reserved for refractory symptoms. During these treatments, a specialist will use a needle to inject a mixture of pain medicine and steroids directly into the joint space. Temporary pain alleviation from injections can last weeks to months.
- Surgery: – Often considered a treatment of “last resort”, surgeries can either decompress pressure on the cord or nerves (such as a discectomy or laminectomy) or stabilize the spine (fusion).
Sources
Katz JN, Zimmerman ZE, Mass H, Makhni MC. Diagnosis and Management of Lumbar Spinal Stenosis: A Review. JAMA. 2022 May 3;327(17):1688-1699. doi: 10.1001/jama.2022.5921. PMID: 35503342.
Jensen RK, Jensen TS, Koes B, Hartvigsen J. Prevalence of lumbar spinal stenosis in general and clinical populations: a systematic review and meta-analysis. Eur Spine J. 2020 Sep;29(9):2143-2163. doi: 10.1007/s00586-020-06339-1. Epub 2020 Feb 24. PMID: 32095908.