Anterolisthesis and slipped disc are two common spinal conditions that can cause back pain and discomfort. However, these terms refer to distinct medical conditions with different underlying causes and treatments. In this article, we will explore the differences between anterolisthesis and a slipped disc to help patients better understand their condition and seek appropriate medical care.
Defining Anterolisthesis and Slipped Disc
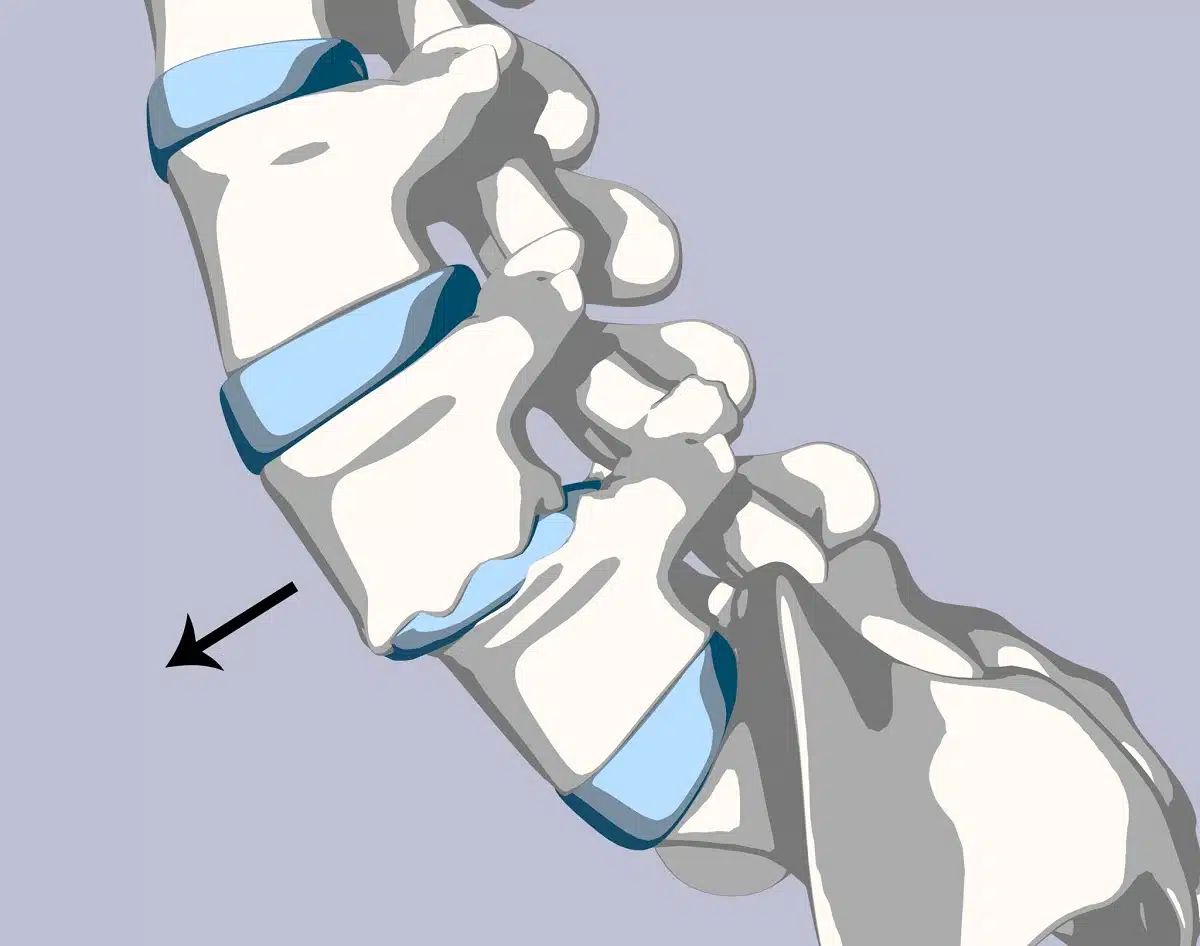
Anterolisthesis is a spinal condition characterized by the forward displacement of one vertebra over another. This condition occurs when there is instability in the spinal segment, leading to the misalignment of adjacent vertebrae. The severity of anterolisthesis is graded from 1 to 4, with grade 1 indicating a 25% slippage and grade 4 indicating a 100% slippage.
On the other hand, a slipped disc, also known as a herniated or ruptured disc, is a condition that affects the intervertebral discs of the spine. Intervertebral discs act as cushions between the vertebrae, allowing flexibility and shock absorption. When a disc herniates, its inner gel-like material protrudes through a tear in the disc’s outer layer, potentially compressing nearby nerves and causing pain.
Distinguishing Characteristics
The primary difference between anterolisthesis and a slipped disc lies in their underlying causes and mechanisms. Anterolisthesis is often a result of degenerative changes in the spine, such as age-related wear and tear, osteoarthritis, or spinal instability due to trauma. It can also be caused by congenital conditions affecting the vertebrae’s shape or alignment.
On the other hand, a slipped disc often occurs due to sudden trauma, repetitive strain, or improper lifting techniques, which cause excessive pressure on the discs, leading to herniation. While anterolisthesis involves the vertebrae’s displacement, a slipped disc involves the protrusion of disc material into the spinal canal.
Symptoms and Diagnosis
Both anterolisthesis and a slipped disc can cause similar symptoms, including back pain, numbness, tingling, and weakness in the affected area. However, specific symptoms may vary depending on the location and severity of the condition.
To diagnose these conditions, healthcare professionals may perform a thorough physical examination, review the patient’s medical history, and order imaging tests such as X-rays, CT scans, or MRIs. These tests help visualize the spine’s alignment and identify any vertebral slippage or disc herniation.
Treatment Options
Treatment for anterolisthesis and a slipped disc differs due to their distinct causes. In mild cases of anterolisthesis, conservative treatments like rest, physical therapy, and anti-inflammatory medications may be sufficient to manage symptoms and promote healing. However, severe cases or those causing nerve compression may require surgical intervention, such as a fusion, to stabilize the spine and relieve pressure on the nerves.
For a slipped disc, conservative treatment options may include rest, pain medication, physical therapy, and epidural injections to reduce inflammation and pain. In cases where conservative measures fail to provide relief, surgery such as a discectomy, may be recommended to remove the herniated disc material and alleviate pressure on the nerves.
The Takeaways
Anterolisthesis and a slipped disc are distinct spinal conditions with different causes and treatments. Anterolisthesis involves the forward displacement of one vertebra over another, often due to degenerative changes or spinal instability, while a slipped disc is characterized by the herniation of disc material due to sudden trauma or strain. Proper diagnosis and treatment are crucial for managing symptoms effectively and improving patients’ quality of life. If you experience persistent back pain or other symptoms, it’s essential to consult a healthcare professional for a comprehensive evaluation and personalized treatment plan.